The cost of dialysis in New York City for 2026 is extremely high, but most patients do not pay the full amount. The billed charge for a single hemodialysis session can range from $800 to $2,500, translating to an annual “sticker price” of **$300,000 to $500,000+. However, with Medicare, Medicaid, or private insurance, out-of-pocket costs are typically capped. Most insured patients will pay co-pays, coinsurance, and premiums, with annual costs often ranging from $2,000 to $10,000+ depending on their plan.
A diagnosis of End-Stage Renal Disease (ESRD) requiring dialysis is life-altering, both medically and financially. In a high-cost environment like New York City, understanding the expenses associated with this life-sustaining treatment is critical for patients and their families. This comprehensive guide for 2026 will demystify the complex pricing of dialysis, breaking down the staggering “list prices” versus the actual out-of-pocket costs most patients face. We will explore how Medicare, Medicaid, and private insurance cover treatment, detail additional expenses, and provide resources for financial assistance to help you navigate this challenging journey without being overwhelmed by medical bills.
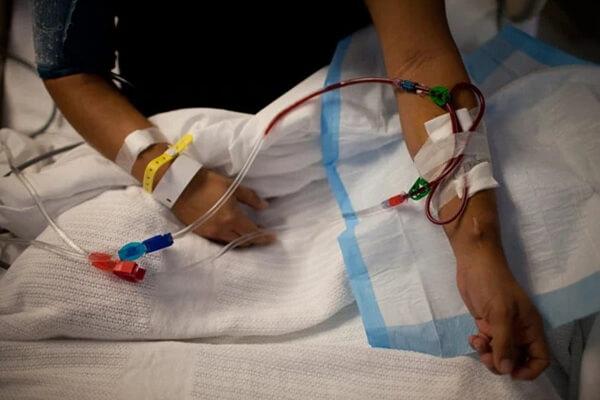
Dialysis Cost in New York NY
Getting dialysis treatment in New York City can be expensive without insurance, but most patients use Medicare, Medicaid, or private insurance to reduce out-of-pocket costs. The price depends on the type of dialysis, the clinic, and whether treatment is done in a hospital or outpatient center. For 2026, the average self-pay cost per dialysis session in NYC ranges from $350 to $900.
For hemodialysis at a dialysis center, which is the most common type, the typical cost is about $400 to $700 per session for uninsured patients. Most patients require three sessions per week, which means the monthly cost can range from $4,800 to $8,400, and the annual cost can exceed $55,000 to $100,000 without insurance. Hospital-based dialysis is usually more expensive and may reach $800 to $1,200 per session, especially if emergency care or overnight monitoring is involved.
For peritoneal dialysis (home dialysis), costs are often slightly lower per treatment but include supplies, equipment, and training. In NYC, self-pay peritoneal dialysis typically averages $3,000 to $5,500 per month, depending on the type of solution used and delivery frequency. Some patients prefer home dialysis because it offers flexibility and fewer clinic visits.
If you have Medicare, it usually covers about 80% of dialysis costs, and secondary insurance or Medicaid may cover the remaining portion. Many eligible patients pay little or nothing out of pocket once coverage is active. Emergency dialysis for uninsured patients in hospitals can still be very costly.
Overall, you should budget $400–$700 per session for outpatient dialysis, $800–$1,200 for hospital dialysis, and $3,000–$5,500 per month for home dialysis if paying privately in New York City.
Understanding Dialysis: Treatment Types and Frequency
Dialysis performs the function of failing kidneys, filtering waste and excess fluid from the blood. There are two primary types, both requiring a significant time commitment.
Hemodialysis (HD): The most common form, where blood is filtered through a machine. This is typically done at a dialysis center three times a week for about four hours per session. Some patients may qualify for home hemodialysis.
Peritoneal Dialysis (PD): This method uses the lining of the patient’s own abdomen (the peritoneum) as a filter. A dialysis solution is introduced and drained multiple times a day, often overnight. This is primarily done at home, offering more flexibility.
The frequency and type of treatment are major drivers of the total cost.
Breaking Down the “Sticker Price” of Dialysis
Breaking down the “sticker price” of dialysis helps explain why dialysis appears so expensive in New York City and what you are actually paying for when you see a bill. The published or “sticker” price of a single dialysis session in NYC often ranges from $400 to $1,200 per treatment, depending on whether it is performed at an outpatient dialysis center or inside a hospital.
This price includes multiple cost components bundled together, such as the use of specialized dialysis machines, disposable filters and tubing, sterile fluids, nursing staff, technician support, physician oversight, laboratory testing, infection control supplies, and facility operating costs like rent, utilities, and regulatory compliance. Hospitals usually charge more than independent dialysis clinics because of higher staffing levels, emergency readiness, and overhead expenses.
Medications given during treatment, such as blood pressure stabilizers, iron, or clot-prevention drugs, may also be included or billed separately. For home dialysis, the sticker price reflects monthly delivery of supplies, equipment rental, training sessions, and ongoing clinical monitoring, which can total $3,000 to $5,500 per month without insurance.
While these prices look extremely high on paper, most patients do not pay the full sticker price because Medicare, Medicaid, or private insurance negotiates much lower rates and covers a large portion of the cost, significantly reducing out-of-pocket expenses for eligible patients.
The Role of Insurance: Medicare, Medicaid, and Private Plans
The role of insurance — Medicare, Medicaid, and private plans — is critical in making dialysis affordable in New York City, because the full sticker price of treatment is extremely high for most patients. Dialysis is considered a life-sustaining treatment, so federal and state programs provide strong coverage protections that significantly reduce out-of-pocket costs for eligible patients.
Medicare is the primary payer for most dialysis patients in the U.S., even for people under age 65 who have end-stage kidney disease. Once enrolled, Medicare typically covers about 80% of approved dialysis costs, including in-center hemodialysis, home dialysis supplies, lab tests, and many dialysis-related medications. Patients are usually responsible for the remaining 20%, unless they have secondary insurance or Medicaid to cover that portion. In NYC, many patients pay very little monthly once Medicare is active, although there may be deductibles and co-insurance depending on the plan and timing of enrollment.
Medicaid helps low-income residents and often acts as secondary insurance for people who already have Medicare. If you qualify for Medicaid in New York, it may cover most or all remaining out-of-pocket costs such as co-pays, transportation to dialysis centers, medications, and home dialysis supplies. For uninsured individuals who meet income guidelines, Medicaid enrollment can dramatically reduce or eliminate dialysis expenses, making long-term treatment financially manageable.
Private health insurance plans through employers or the Marketplace also cover dialysis, but cost sharing varies by plan. Patients may face deductibles, co-insurance, and out-of-pocket maximums that can still be several thousand dollars per year. Some private plans coordinate benefits with Medicare after a waiting period, which can lower long-term costs. Coverage usually includes clinic dialysis, home dialysis equipment, and prescribed medications, but prior authorization and network restrictions may apply.
Overall, insurance coverage is what transforms dialysis from a potential $50,000–$100,000+ annual expense into a manageable or low-cost treatment for most patients in NYC. If you’d like, I can also explain how to apply for Medicare for dialysis, Medicaid eligibility in New York, or how to estimate your personal out-of-pocket costs based on your insurance situation.
Financial Assistance Programs and Resources
Financial assistance programs and resources play an important role in helping dialysis patients in New York City manage treatment costs, especially for those who are uninsured, underinsured, or facing financial hardship. Many dialysis clinics work directly with social workers who help patients apply for Medicare, Medicaid, and supplemental insurance programs, ensuring coverage starts as quickly as possible after diagnosis. For patients who are not immediately eligible for government insurance, nonprofit organizations and charitable foundations often provide temporary financial support to help cover treatment costs, medications, transportation, and insurance premiums.
Several national kidney foundations and patient assistance programs offer grants or co-pay assistance for dialysis-related expenses, including prescription drugs, travel to dialysis centers, and emergency medical needs. Some programs also help pay for insurance deductibles and monthly premiums, which can significantly reduce out-of-pocket burden for families. In New York, local hospitals and nonprofit health networks may offer charity care programs or sliding-scale discounts based on income, especially for uninsured patients receiving hospital-based dialysis.
Transportation assistance is another valuable resource in NYC, as many patients require dialysis three times per week. Medicaid transportation benefits, community shuttle services, and nonprofit ride programs can help reduce travel costs and missed appointments. Additionally, patients who choose home dialysis may qualify for utility assistance programs that help offset higher electricity and water usage related to equipment operation.
Overall, combining insurance coverage with nonprofit assistance, hospital financial aid programs, and transportation support can make long-term dialysis financially manageable in New York City. If needed, dialysis clinic social workers are usually the best starting point to connect patients with the right financial resources and application support.
Frequently Asked Questions (FAQ)
Does Medicare cover 100% of dialysis costs?
No. Medicare Part B covers 80% of the approved amount for dialysis after you meet the annual Part B deductible. You are responsible for the remaining 20% coinsurance unless you have a supplemental Medigap policy or Medicaid.
How much does dialysis cost without insurance?
Without insurance, a patient would be billed the full “sticker price” of $300,000 to $500,000 per year. This is financially catastrophic for almost all individuals. It is crucial to immediately apply for Medicare, Medicaid, or financial assistance through a dialysis clinic social worker.
Is home dialysis cheaper than in-center dialysis?
For the healthcare system, home dialysis (either PD or HHD) is generally less expensive than in-center care. For the patient, the out-of-pocket costs are often similar, as they are determined by insurance co-pays and deductibles. However, home dialysis can save significant money on transportation and time.
What is the 30-month coordination period for dialysis?
This is a rule for patients who have private group health insurance when they start dialysis. For the first 30 months, the private insurance is the primary payer and Medicare is secondary. After 30 months, Medicare becomes the primary payer.
Can I get help paying my Medicare premium for dialysis?
Yes. Programs like the American Kidney Fund (AKF) and Medicare Savings Programs (through Medicaid) can provide grants or assistance to help eligible individuals pay their Medicare Part B premiums, deductibles, and coinsurance.